Are you feeding your Migraine?
Food and migraine is a popular and sometimes confusing subject for my patients.
In this article I discuss food-related disorders such as Coeliac disease, Irritable Bowel Syndrome, Wheat Allergy and Gluten Sensitivity and their relationship with migraine headache.
I discuss how migraine headache, a neurological disorder, can be considered a result of a hyper-active nervous system and the role food plays in this relationship. I would appreciate your feedback on whether this explanation makes sense to you.
Quick Migraine review
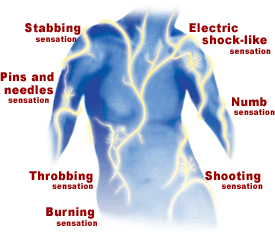
Migraine is a genetic, neurological, life-long condition. You inherit your migraine brain from your parents. Your migraine brain contains nerves that are better at producing headache than a non-migraine brain. Certain things, like stress and fatigue, make these nerves even more capable of producing headache. These kinds of things are called migraine triggers. Certain foods can be one of the triggers that sensitise and switch on your migraine nerves and produce the pain of a headache.
Food as a migraine trigger
20% of migraineurs have a definite food trigger; when they eat a certain food they are guaranteed a migraine. The most common ones are red wine, cheese and chocolate. Some argue it is related to nitrates and phosphates present in these foods. Are there certain foods that trigger your migraine? Most people who have a definite food trigger have already worked this one out. If you are still at a loss, try keeping a food diary to help you figure out if your food intake is related to your headache and migraine pattern.
Skipping meals
American researchers found that skipping meals was one of the most common triggers for migraine. Going for periods of time without sufficient food and water intake stresses your body, sensitises your nervous system and is quite likely to switch on your migraine nerves giving you a headache.
This is a migraine trigger you have complete control over. Look after your body as you would look after a small child. Ensure regular food and water intake.
Food, the Nervous System and Migraine
Central to understanding migraine, is the concept of a genetically determined, hyper-excitable nervous system. A person with migraine has a hypersensitive nervous system that “over-reacts” to certain stimuli such as stress, fatigue, weather changes, certain foods etc. This “over-reaction” switches on their migraine nerves and produces headache.
Here we are examining if certain foods can push the body and nervous system further into a heightened state of excitability where the migraine nerves are more easily switched on producing headache. We are going to focus on specific food-related diseases which have strong links with migraine.
Coeliac Disease, Irritable Bowel Syndrome, Gluten Sensitivity and Wheat Allergy are disorders where food interacts with the person’s disease genes, and combined with a hyper-excitable nervous system produces the symptoms of the disease.
Migraine is more prevalent in people with these diseases compared to the general population. These diseases can remain undiagnosed and untreated for long periods of time. Recognition of the prevalence of these diseases in people with migraine is very important. The presence of these diseases in a person with migraine can be the predominant factor that continues to sensitise an already hyper-excitable nervous system, continuously stimulating their migraine nerves to produce headache.
What is Coeliac Disease?
Coeliac disease is an inherited auto-immune disease where people have a reaction in their intestines to gluten, which reduces their body’s ability to absorb food nutrients. These individuals experience digestive complaints, like diarrhoea, inability to gain weight, and other problems related to poor nutrition such as anaemia, decreased bone density and dermatological changes. These classic symptoms are now being challenged in the literature reporting that up to 70% of females with coeliac disease do not present with gastro-intestinal symptoms but more so; headache, muscle aches and pains, tingling in hands and feet and other neurological symptoms.
The diagnosis of Coeliac disease is made by testing for specific antibodies and a biopsy of the small intestine but these tests are not 100% reliable. There is a greater prevalence of Coeliac Disease in migraine patients than in the general population, and there are some studies to support, that when these people adopt a gluten-free diet, their symptoms, which include migraine headaches, improve.
What is Irritable Bowel Syndrome?
Irritable Bowel Syndrome is a bowel disorder, characterised by recurrent episodes of abdominal pain and discomfort, with marked changes in bowel habits. This can occur in response to ingestion of specific foods, or similarly to migraine, it may not have a definite pattern. Both IBS and migraine have strong links with anxiety and stress. As with migraine, body function returns to normal in between attacks and there is no link to increased risk of other diseases.
What is Gluten Sensitivity and Wheat Allergy?
Gluten sensitivity is an abnormal response to ingesting gluten i.e. stomach complaints, headaches, with resolution of these symptoms on a gluten-free diet. Gluten sensitivity is not linked with a higher risk for other diseases. The only way to test for gluten sensitivity is to adopt a gluten-free diet and assess symptom responses. Wheat allergy is an allergy to wheat, improved by avoiding wheat. Avoiding other gluten-containing foods, like rye, barley and oats, is not necessary.
The Nervous System and Migraine
All of these diseases demonstrate an exaggerated response of the auto-immune and nervous system on ingestion of certain foods. The stimulation of the auto-immune system, where the body cells attack themselves and then return to normal after the event, further sensitise an already hyper-active nervous system.
If you have Coeliac Disease, Irritable Bowel Syndrome, Gluten Sensitivity or Wheat Allergy and continue to eat food that aggravates your disorder, you place your body under continual distress. This continual distress sensitises your nervous system. A sensitised nervous system is more likely to fire and switch on your migraine nerves producing headache.
Is there a place for a Migraine Diet?
The first rule of a migraine diet is to ensure regular food and water intake. The second is avoidance of known migraine food triggers which for those who have them, is already being done.
There is currently insufficient evidence to recommend that all migraine patients should adopt a gluten-free diet. However, if you have, or suspect you have a food-related disorder such as; Coeliac Disease, Irritable Bowel Syndrome, Gluten Sensitivity or Wheat Allergy it is recommended that you consult your GP or health professional and commit yourself to a 3-month food trial while monitoring your symptoms.
Symptoms that may alert you to the possibility that you might have a gastro-intestinal disorder include; stomach pain and cramping, change in bowel habits, diarrhoea, constipation, stomach bloating and swelling, chronic tiredness, nausea, vomiting, family history of Coeliac disease.
As a clinical guideline if a patient presents with stomach problems as part of their migraine picture, i.e. stomach discomfort before, during or after their migraine headache I would alert them to the possibility that their food intake may be playing a role in their migraines and provide them with options and further education. Feel free to contact me for any more information on info@proactivephysio.ie or 00353851670574.
References:
1. Andreas-Rothrock, D, King, W, Rothrock, J (2010) An analysis of migraine triggers in a clinic-based population Headache: the Journal of Head and Face Pain 50 (8) 1366-1370
2. Cady, RK, Farmer, K, Dexter, JK, Hall, J (2012) “The Bowel and Migraine: Update on Celiac Disease and Irritable Bowel Syndrome” Curr Pain Headache Rep 16:278-286
3. Dimitrova, AK, Ungaro RC, Lebwohl, B, Lewis SK, Tennyson, CA, Green, MW, Babyatsy, MW, Green, PH (2013) “Prevalence of Migraine in Patients with Celiac Disease and Inflammatory Bowel Disease” Headache 53:344-355
4. Lionetti, E, Francavilla R, Maiuri, L, Ruggieri, M, Spina, M, Pavone, P, Francavilla, T, Magista AM, Pavone, L (2009) “Headache in Pediatric Patients with Celiac Disease and its Prevalence as a Diagnostic Clue” Journal of Pedatric Gastroenterology and Nutrition 49:202-207
5. Pascual, J, Oterino, A (2010) “IgG-mediated allergy: A new mechanism for migraine attacks?” Cephalalgia 30(7) 777-779
6. Sapone, A, Bai, JC, Ciacci, C, Dolinsek, J, Green, PHR, HAdjivassiliou, M, Kaukinen, K, Rostami, K, Sanders, DS, Schumann, M, Ullrich, R, Viallalta, D, Volta, Umerto, Catassi, C, Fasao, A (2012) “Spectrum of gluten-related disorders: consensus on new nomenclature and classification” BMC Medicine 10:13
7. Wahnschaffe, U, Ullrich, R, Riecken, EO, Schulzke, JD (2001) “Celiac Disease-like abnormalities in a subgroup of patients with Irritable Bowel Syndrome” Gastroenterology 121:1329-1338